

Expert posterior cruciate ligament reconstruction by British-trained ACL PCL surgeon Dr. Mohammad Ashfaq Konchwalla — with over 2,000 knee ligament procedures performed at Medcare Hospital, Dubai. Treating isolated PCL tears and complex multiligament knee injuries.
The posterior cruciate ligament (PCL) is the strongest ligament in the knee — a robust band of tissue running diagonally through the centre of the joint, connecting the femur to the tibia and preventing the tibia from sliding backwards. The PCL is the primary restraint to posterior tibial translation, working in concert with the ACL to provide rotational and multi-directional knee stability. While less common than ACL tears, PCL injuries account for approximately 20% of all knee ligament injuries and are among the most complex and frequently under-diagnosed conditions in sports surgery Dubai. An experienced ACL PCL surgeon is essential to correctly grade the injury and determine the optimal management pathway.
Dr. Mohammad Ashfaq Konchwalla is a British-trained FRCS-certified orthopaedic and sports surgeon with over 2,000 knee ligament procedures to his name — an experienced ACL PCL surgeon in Dubai who assesses and treats the full spectrum of PCL injuries, from isolated Grade I partial tears managed conservatively, to complex Grade III complete PCL ruptures and multiligament knee injuries requiring sophisticated staged surgical reconstruction. His comprehensive approach addresses not just the PCL in isolation, but every associated ligament, meniscus, and cartilage injury — giving patients the best possible chance of full recovery and return to sport.
PCL tears most commonly result from a direct blow to the front of a bent knee — the classic "dashboard injury" in road traffic accidents, or a direct tackle in contact sports. The posterior tibial sag and characteristic clinical signs (Posterior Drawer Test, Quadriceps Active Test) allow accurate bedside diagnosis, confirmed by MRI. Unlike ACL tears, many isolated Grade I and II PCL injuries can be managed successfully without surgery through quadriceps-focused physiotherapy — making accurate grading by an expert PCL surgeon in Dubai critical to appropriate care.
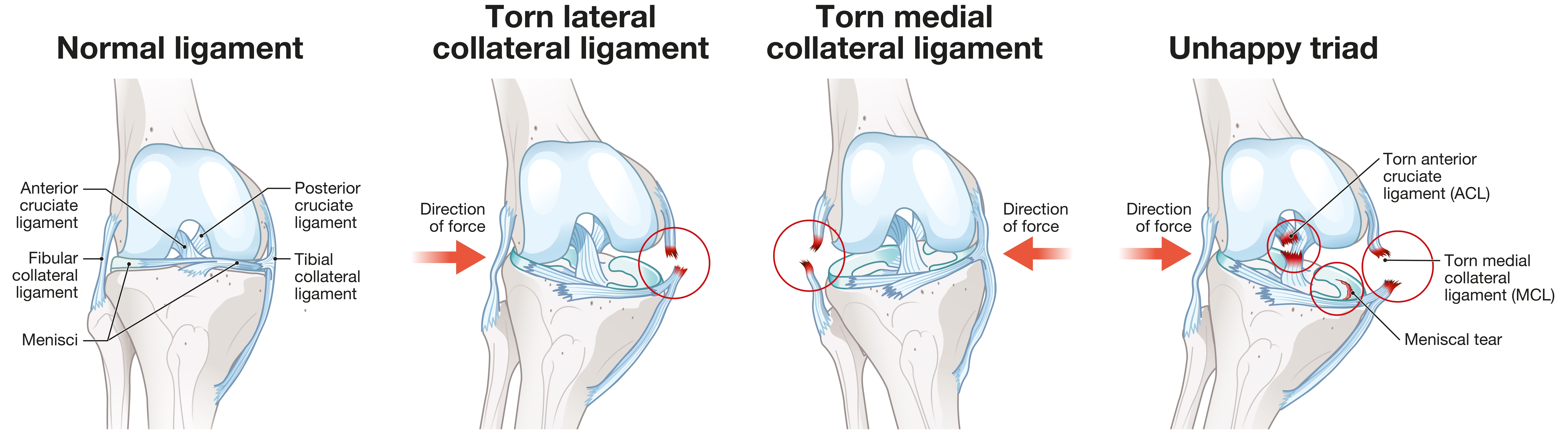
PCL injuries range from partial tears managed conservatively to severe multiligament knee dislocations requiring urgent surgical planning. Select a condition below to learn how Dr. Konchwalla approaches each injury pattern.
Treatment of a PCL tear is tailored to the injury grade, the presence of combined ligament injuries, the patient's activity level, and their goals. As an experienced ACL PCL surgeon in Dubai, Dr. Konchwalla offers the full range of surgical and non-surgical management options and will advise the most appropriate approach at consultation.
Every PCL reconstruction at Medcare Hospital Dubai follows a precise surgical protocol tailored to the patient's injury grade, combined ligament involvement, and graft selection. Click any step to expand details.
Clinical examination (Posterior Drawer Test, Quadriceps Active Test, Sag Sign, Dial Test for PLC). MRI confirms PCL tear, grades the injury, and identifies concurrent ligament, meniscus, and cartilage damage. Vascular assessment if dislocation suspected. Pre-operative physiotherapy optimises quadriceps before surgery.
General or spinal anaesthesia with peripheral nerve block. Patient positioned to allow both arthroscopic portals and, if needed, a posteromedial approach. Thorough joint assessment under anaesthesia confirms laxity patterns. Combined ligament injuries are addressed in the planned sequence.
Arthroscope introduced to confirm PCL rupture, assess both menisci, articular cartilage, and ACL. Any concurrent meniscus tears repaired. Graft harvested through a separate incision — hamstring, patellar tendon, or allograft prepared on the back table to the required diameter and length.
Tibial and femoral tunnels drilled to precisely replicate the native PCL footprint under arthroscopic and fluoroscopic guidance. The tibial inlay technique may be used to avoid the "killer turn" of graft abrasion. Graft passed and tensioned in the correct anatomical position. Posterior capsule protected throughout.
Graft secured with interference screws or cortical buttons at both tibial and femoral ends. If combined ACL, MCL, or PLC injuries are present, these are addressed in the planned sequence during the same anaesthetic. Stability confirmed arthroscopically through full range of motion.
Patients are fitted with a hinged knee brace locked in extension and provided with crutches before discharge. Written aftercare instructions, home exercise programme, and physiotherapy referrals arranged before leaving Medcare Hospital. Neurovascular checks performed before discharge.
PCL rehabilitation is a structured, criterion-based process with a strong emphasis on quadriceps strengthening as the primary dynamic stabiliser of the PCL-reconstructed knee. The brace is worn for 6 weeks to protect graft healing. Progress is guided by strength and functional milestones — not the calendar alone.
British-trained. FRCS-certified. Dubai's specialist ACL PCL surgeon — trusted by athletes and active patients across the UAE and beyond.
The PCL is most commonly injured in high-contact sports and high-energy mechanisms. Dr. Konchwalla tailors both the surgical approach and rehabilitation to each athlete's specific sport demands.
Common questions about PCL surgery in Dubai — answered by Dr. Konchwalla's team at Dubai Sports Surgery.
Book a consultation with Dubai's specialist ACL PCL surgeon — British-trained, FRCS-certified orthopaedic & sports surgery expert. Take the first step toward a full, confident recovery. Appointments available within 48 hours.